During knee arthroscopy, Dr Hutabarat inserts a small fibre optic camera, called an arthroscope, into your knee joint.
The camera displays pictures on a video monitor, and your surgeon uses these images to guide miniature surgical instruments.
Because the arthroscope and surgical instruments are thin, your surgeon can use very small incisions, rather than the larger incision needed for open surgery. This results in less pain for patients, less joint stiffness, and often shortens the time it takes to recover and return to activities.
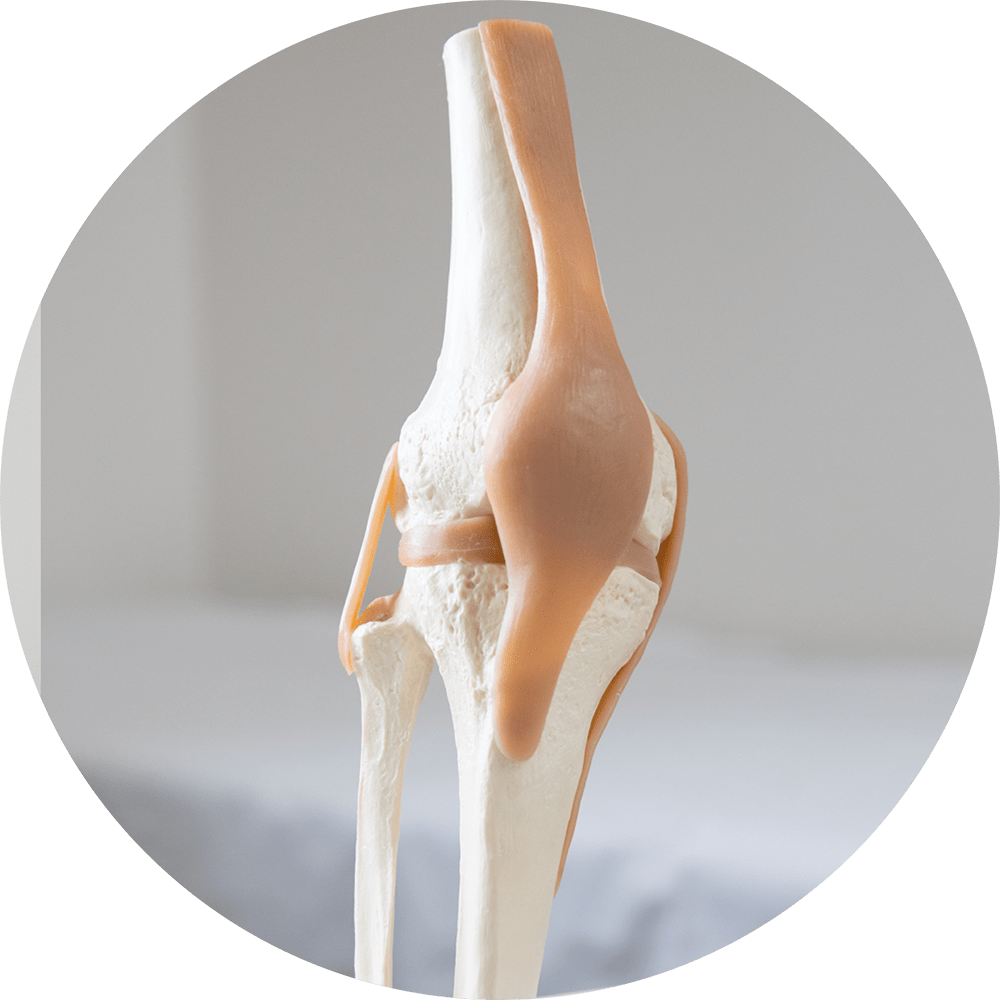
Anatomy
Your knee is the largest joint in your body and one of the most complex. The bones that make up the knee include the lower end of the femur (thighbone), the upper end of the tibia (shinbone), and the patella (kneecap).
Other important structures that make up the knee joint include:
- Articular cartilage. The ends of the femur and tibia, and the back of the patella are covered with articular cartilage. This slippery substance helps your knee bones glide smoothly across each other as you bend or straighten your leg.
- Synovium. The knee joint is surrounded by a thin lining called synovium. This lining releases a fluid that lubricates the cartilage and reduces friction during movement.
- Meniscus. Two wedge-shaped pieces of meniscal cartilage act as “shock absorbers” between your femur and tibia. Different from articular cartilage, the meniscus is tough and rubbery to help cushion and stabilise the joint.
- Ligaments. Bones are connected to other bones by ligaments. The four main ligaments in your knee act like strong ropes to hold the bones together and keep your knee stable. The two collateral ligaments are found on either side of your knee. The two cruciate ligaments are found inside your knee joint. They cross each other to form an “X” with the anterior cruciate ligament in front and the posterior cruciate ligament in back.
When is a Knee Arthroscopy Recommended?
Your doctor may recommend knee arthroscopy if you have a painful condition that does not respond to nonsurgical treatment. Nonsurgical treatment includes rest, physical therapy, and medications or injections that can reduce inflammation.
Knee arthroscopy may relieve painful symptoms of many problems that damage the cartilage surfaces and other soft tissues surrounding the joint.
Common arthroscopic procedures for the knee include:
- Removal or repair of a torn meniscus
- Reconstruction of a torn anterior cruciate ligament
- Removal of inflamed synovial tissue
- Trimming of damaged articular cartilage
- Removal of loose fragments of bone or cartilage
- Treatment of patella (kneecap) problems
- Treatment of knee sepsis (infection)
Complications
The complication rate after arthroscopic surgery is very low. If complications occur, they are usually minor and are treated easily.
Possible postoperative problems with knee arthroscopy include:
- Infection
- Blood clots
- Knee stiffness
- Accumulation of blood in the knee
Recovery
After surgery, you will be moved to the recovery room and should be able to go home within 1 or 2 hours. Be sure to have someone with you to drive you home and check on you that first evening. While recovery from knee arthroscopy is faster than recovery from traditional open knee surgery, it is important to follow your instructions carefully after you return home.
-
Pain Management
After surgery, you will feel some pain. This is a natural part of the healing process. Your doctor and nurses will work to reduce your pain, which can help you recover from surgery faster. Medications are often prescribed for short-term pain relief after surgery. Many types of medicines are available to help manage pain, including opioids, non-steroidal anti-inflammatory drugs (NSAIDs), and local anaesthetics. A combination of these medications may improve pain relief, as well as minimise the need for opioids.
Be aware that although opioids help relieve pain after surgery, they are a narcotic and can be addictive. It is important to use opioids only as directed by your doctor. As soon as your pain begins to improve, stop taking opioids. Talk to the orthopaedic team if your pain has not begun to improve within a few days of your surgery.
-
Medications
In addition to medicines for pain relief, you may also be recommended medication such as aspirin, clexane or Xarelto to lessen the risk of blood clots.
-
Swelling
Keep your leg elevated as much as possible for the first few days after surgery. Apply ice as recommended by your doctor to relieve swelling and pain.
-
Dressing Care
You will leave the hospital with a dressing covering your knee. Keep your incisions clean and dry. Instructions will be given which will tell you when you can shower or bathe, and when you should change the dressing (usually 1 week). The orthopaedic team will see you in the office a few days after surgery to check your progress, review the surgical findings, and begin your postoperative treatment program.
-
Bearing Weight
Many patients need crutches or other assistance after arthroscopic surgery. In most cases you will be able to weight bear. If thing differ, Dr Hutabarat will tell you when it is safe to put weight on your foot and leg. If you have any questions about bearing weight, please call the hospital or the rooms.
-
Rehabilitation Exercise
You should exercise your knee regularly for several weeks after surgery. This will restore motion and strengthen the muscles of your leg and knee. Therapeutic exercise will play an important role in how well you recover. A formal physical therapy program may improve your final result.
-
Driving
Dr Hutabarat will discuss with you when you may drive. Typically, patients are able to drive from <1 to 3 weeks after the procedure.
Frequently Asked Questions (Knee Arthroscopy)
-
How long am I in for?
Just the for part of the day. There is a bit of time waiting around before and after the surgery so allow about 4 hours
-
How much does it cost?
Surgeons charge different fees for many different reasons so it pays to ask around and get other opinions! We do a quote for all our patients. Don’t be afraid to ask questions. We like questions and are happy to answer them.
-
When can I return to sport?
This depends upon the sport, the level of its intensity and the damage in your knee. We want to get you back as soon as we can and will tailor your return to your situation.
-
When can I get it wet? Or swim? Or surf?
Generally wounds need to stay dry for two weeks and then we may give a bit more time as a precaution. Dr Hutabarat has his personal method of an early return to the ocean if it’s pumping. This can be discussed on a case by case basis.
-
What about timing for my holidays/travel?
This is a very important question! Its best to allow 3 weeks before a trip… again it depends on the situation.
Have a question or inquiry or looking for some more information about our services, get in touch and we will be happy to assist.